Schizophrenia; The Hallmark Of Psychiatric Illnesses | Pathophysiology Of Schizophrenia Disorder
Table Of Interest
Today, you and I will quickly take a look at the topic “Schizophrenia; The Hallmark Of Psychiatric Illnesses | Pathophysiology Of Schizophrenia Disorder“.
This has become necessary as we have sen overtime that several individuals have been searching for topics related to the above topic Schizophrenia; The Hallmark Of Psychiatric Illnesses | Pathophysiology Of Schizophrenia Disorder.

However, if you are among those that have been searching for answers to [pathophysiology of schizophrenia diagram, pathophysiology of schizophrenia disorder, psychopathology of schizophrenia, etiology of schizophrenia, schizophrenia spectrum and other psychotic disorders dsm 5, schizophrenia symptoms, dsm 5 schizophrenia diagnosis, pathophysiology of schizophrenia nursing, Schizophrenia; The Hallmark Of Psychiatric Illnesses | Pathophysiology Of Schizophrenia Disorder], then you can see that you are not the only one.
Nonetheless, you shall get all this information right here on this blog.
Schizophrenia; The Hallmark Of Psychiatric Illnesses | Pathophysiology Of Schizophrenia Disorder

Crazy. That’s the word which is commonly used for people who appear bizarre, walking along the street with no shoes or slippers and sleep anywhere they can lie their head onto.
It’s no mystery that some people who have certain symptoms of psychiatric illness would act differently than what is accepted by the social and cultural norm.
Stigma has always been the reason why people are generally scared to seek help from a medical professional.
Mental disturbances have always been associated with weakness, self-blame, witchcraft and demon’s possession. In the past, people who are perceived to act differently from the others are thought to have been possessed by a demon.
A lot of rituals has been performed including exorcism in the past and the most extreme one is to drill a hole in a patient skull to let the demon inside his/her head out.
Of course, without proper setting and technique, this procedure is fatal. Damn it, blame it on the demon! I just drilled a hole in his head to let the demon out.

Schizophrenia has always been the hallmark of psychiatric illnesses.
Talking to themselves, inappropriate facial expression, slow movement, catatonia, hallucination, delusion and bizarre appearance; all of them describe the abnormality in a few domains in the brain which affect functionality and judgement.
Those domains are:
I think most of the terminologies being used above are self-explanatory except for affect. Affect is the experience of emotion, it serves as important tools of social interaction to predict an individual preference.
For example, when communicating with others, the general rule of facial expression will tell you, if a person smile, they can be thought as comfortable with the topic of discussion; sour face would reflect otherwise.
Affect usually can be represented in three components:

In an individual with schizophrenia, they generally have blunted affect.
Their facial, vocal and gestural might be the same for most of the emotions they were having.
This imposed some sort of difficulty for them to perform in a social interaction which makes it simple and logical for them to just being alone, avoiding social interaction.
Some people with schizophrenia do have an affect, but it is inappropriate.
People usually laughing when they were happy and cry when they were sad but if there is some sort of pathological changes which can affect the integrity of physiological affect, it could be the other way around.
Their behaviour might be deemed unacceptable by the community due to the bizarreness of responses towards specific stimuli; for example, the news about someone dying should not be received with laughter.
The disruption in the majority if not all of the domains of social function in an individual with schizophrenia has made this disease quite disabling.
They were often fired from their job, being denied the opportunity to apply for a certain position, normal social interaction, the opportunity to buy a house in a safe housing area and some medical benefits which can be provided by certain insurance companies.
Tough luck!

Before the term, “schizophrenia” was coined by a Swiss psychiatrist, people who showed the symptoms which can be related to schizophrenia are thought to have an early onset of dementia.
This is attributed to a German psychologist name Emil Kraepelin way back in the 1800s.
He proves that people who are presented with the symptoms related to schizophrenia are not possessed by a demon or anything, they just were having a series of pathological changes which lead to a condition called “dementia praecox” or also known as premature madness.
It seems plausible but Kraepelin never specified the symptom’s list which can be a guide to diagnosed people with dementia praecox.
In 1911, Eugen Bleuler has come up with a pattern which could be used to diagnose people with the condition equivalent to what has been proposed by Kraepelin.
This illness is usually presented in 4 disorganisation themes:
This concept expands the hypothesis made by Kraepelin and Bleuler eventually create the term “schizophrenia” which originated from a Greek word which meant “split mind”. Before you said anything, this is a different concept from Dissociative Identity Disorder (DID) or commonly known as the Multiple Personality Disorder.
Through a series of discovery, people started to understand bit by bit the psychopathological features of schizophrenia and all of the required symptoms to diagnosed were recorded in the Diagnostic and Statistical Manual of Mental Disorders (DSM) which is an important tool used by the clinician.
I would not bore you with details of the latest issue of DSM for diagnosing schizophrenia, you can pretty much find it on the internet.
Etiology of disease

For laymen out there, aetiology is the causation of a disease process.
What causes people to get schizophrenia? Well, multiple studies have shown that schizophrenia started around late adolescence to early adulthood.
This is the timeline which affects the individual the most, psychologically speaking, as it is a crucial time for:
- People to live independently
- Searching for personal preferences (identity)
- Moulding their own personality (maturation)
- Develop a healthy heterosexual relationship within a community
Any disruption which leads to schizophrenia can cost individual performances in education, social interaction and personality. There is no discrepancy between gender but earlier onsets were common among men compared to women.
Should you be relieved if you have passed early adulthood without any symptoms which indicate you were having schizophrenia? The answer would be no.
Schizophrenia can be caused by organic diseases and substance abuse. People who have been diagnosed with schizophrenia when they were past 40 have a higher probability to be caused by organic diseases.

There are three factors which have been identified to cause schizophrenia:
Genetic attribution has been an important factor which is correlated with a high morbidity rate provided the disease runs in the family. In the general population, the risk of someone getting schizophrenia was 1%.
The chance seems quite low but the number didn’t take any familial factors into account.
See Articles Others Are Reading
- Study Abroad In Canada | See Top 10 scholarships To Study Abroad In Canada
- 2018 International Masters Scholarship at the University Of Oulu
- Fully funded Singapore International Scholarship 2019
- Fully Funded Duke University International scholarship 2019
- Kings College London International Scholarship
If either parent or any siblings have schizophrenia, there is a 10% chance for you to get schizophrenia later as well.
If both parents have schizophrenia, the probability scale up to 40%.
If any of your blood relatives (second-degree relatives) have schizophrenia, the probability for you to develop schizophrenia would be 3%. Monozygotic and dizygotic twin study have proved the probability of 50% and 10% respectively if either one of the twins has schizophrenia.

Environmental factor usually won’t help much.
A few studies conducted in the past has disproved the role of environment in accelerating or preventing the onset of schizophrenia in a genetically susceptible people.
A child with siblings that have schizophrenia would have a high probability to experience the onset of the disease at the same age as the other siblings despite the difference in the environment.
Apart from the genetical component, the biochemical component is an important aspect of the disease’s aetiology as well.
There are generally four hypotheses which have been made to explain schizophrenia:
- Dopamine hypothesis
- Serotonin hypothesis
- Glutamate hypothesis
- Gamma-aminobutyric acid (GABA) hypothesis
All of the hypotheses were derived from the mechanism of action of the pharmacological agent of schizophrenia. Some hallucinogen has been found to cause the symptoms which resemble schizophrenia by elevating the serotonin activities.
This lead to the development of atypical antipsychotics which act upon the serotonin receptor that improves the signs and symptoms of schizophrenia. It is difficult to pinpoint the exact cause of schizophrenia as it is multifactorial but you get the gist.
Some of the people with schizophrenia produce too much dopamine in his/her system so an antipsychotic which acts as a dopamine receptor antagonist can be used.
This would improve the signs and symptoms of the disease process.
Negative symptoms such as reduced cognitive function are usually caused by brain abnormalities.
The most common finding of the brain scan of people with schizophrenia revealed an enlarged sulcus and ventricle which is associated with a small size thalamus and brain atrophy.
The other explanation for the negative symptoms would be a reduced blood flow to the prefrontal cortex known as the hypofrontality.
Pre and perinatal causes of schizophrenia are not common but some studies indicate both of them are one of the most important factors which can lead to schizophrenia.
Birth trauma and complications were common and the risk for an individual to be diagnosed with schizophrenia can be caused by:
- Birth asphyxia
- Gestational diabetes
- Maternal haemorrhage
- Low birth weight
- Lower segment cesarean section
- Congenital infection
Psychosocial factors are some of the most common reason why people who are genetically predisposed to schizophrenia developed the ailment. Usually, the first appearance of schizophrenia symptoms was preceded by stressful events.
Normal people (people who are not genetically predisposed) usually would respond differently compared to someone who is genetically predisposed.
The feeling of overwhelm was exaggerated and long before they knew it, they were diagnosed with schizophrenia. There are two common problems faced by people before were diagnosed with the ailment:
- Problems in the family
- Problems in social interaction

People who are diagnosed with schizophrenia were often single.
They like to live by themselves because there was lack of social demand making them comfortable.
If there is some sort of thing which involved social interaction, they will become anxious and restless. High express emotion (EE) environment is another important psychosocial component which could cause schizophrenia. High EE would include:
Wew. There are so many factors, isn’t it? All of this factors could interact with one another which would increase the probability of someone getting schizophrenia.
The Outcome Paradox

There are approximately 22 million people around the globe who has been diagnosed with schizophrenia and the number keep on increasing. Schizophrenia has a variable treatment outcome.
The outcome can be simplified into a set of probability called a rule of thirds:
- 1/3 of people would completely recover (good prognosis)
- 1/3 would improve over time (fair prognosis)
- 1/3 would not respond well to treatment (poor prognosis)
Among the 22 million, it was estimated 50% of them were not treated for their condition.
This is a major concern since schizophrenia is a disabling ailment and the commonest age range usually affected were between late adolescence and young adult (critical period for moulding personality).
For most of the diseases, more money equal to better treatment regimens which would equal to a better outcome. For schizophrenia, the outcome is different.
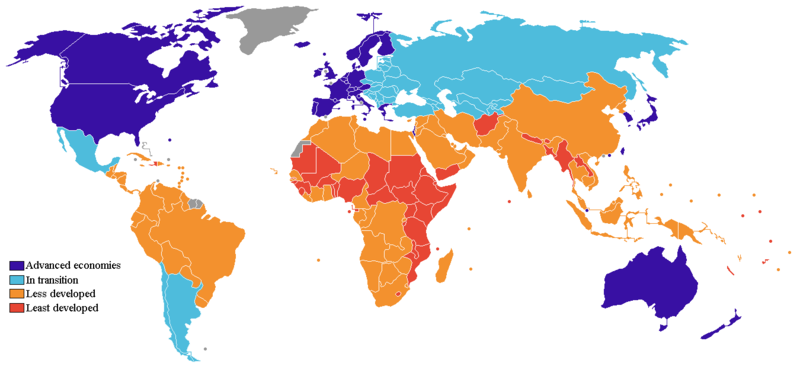
40 years ago, a study which has been conducted in a few developing countries has shown that the outcome of treatment for a patient with schizophrenia in developing countries was much better compared to its counterpart despite the lack of resources.
The patients were reported to have fewer hallucinations, better cognitive and social functions and less disorganized behaviours.
However, the outcome of the study was considered inaccurate since there is no standardised structure for diagnostic criteria and method of assessment.
A few years later, the World Health Organisation has conducted three international studies which could serve as standardised research methods for comparing the respond of treatment for a patient with schizophrenia in developing and developed countries. Those studies were:
- International Pilot Study of Schizophrenia (IPSS)
- International Study of Schizophrenia (ISoS)
- Determinants of Outcomes of Severe Mental Disorders (DOSMeD)
There are nine countries (India, Colombia, Nigeria, Taiwan, Denmark, the United Kingdom, the United States of America, Soviet Union, Czechoslovakia) which involved in IPSS with a total of 1,202 patients. The outcome of the treatment would be measured based on three domains:
- Level of social impairment
- Type of remission
- The frequency of psychotic symptoms
This study was conducted for five years and after that period, it was found that India (42%) and Nigeria (33%) have the most success in terms of treatment outcome of schizophrenia patient.
The other developed countries scored less than 10% except for the United States of America which has a 17% success rate in treating patients with schizophrenia.

DOSMeD and ISoS yield similar outcomes.
The rate of recovery was higher in the developing countries compared to the developed countries.
Patients in developing countries also were reported to have a longer period of remission compared to patients in developed countries.
This can be caused by a few contributing factors such as stigma and nurturing cultures. In a certain developing country, the difference between psychiatric and non-psychiatric illnesses are not apparent.
This subsequently reduced stigma which would encourage more people to seek treatment hence better treatment outcomes.
This phenomenon is termed the outcome paradox. People with schizophrenia who reside in a developing country have a higher rate of recovery compared to people who live in a developed country.
Conclusion
Living with psychiatric illness is not easy.
Sometimes stigma imposed a greater challenge than the disease process itself.
Even though knowledge on the psychopathology and principle of treatment have improved over time, there are so much to learn about the disease process and how the outcome paradox takes a hold of the treatment outcome.
Most of the studies proving the existence of this paradox but never explain the mechanism of it. Whatever it is, due to the social influence on people with schizophrenia, treating the disease would be difficult for the time to come.
That’s the much we can take on the Topic “Schizophrenia; The Hallmark Of Psychiatric Illnesses | Pathophysiology Of Schizophrenia Disorder”.
Thanks For Reading
Leave a Reply